Health information
Our easy-to-understand information explains symptoms and conditions that affect lots of women.
If you are worried or need medical advice, please speak to your doctor, midwife or healthcare professional.
Use the buttons below to filter by category.

Top tips for managing periods as a teenager
Periods & menstrual health

Who can I trust when learning about my period?
Periods & menstrual health

What is a menstrual cycle?
Periods & menstrual health

15 period mythbusters
Periods & menstrual health

What is pre-eclampsia?
Pregnancy & birth

What is infertility?
Fertility

What is irregular bleeding?
Periods & menstrual health

Your rights at work when you have painful or heavy periods
Periods & menstrual health

What to do if you're feeling dismissed by your healthcare professional
Periods & menstrual health

How to prepare for your doctor’s appointment
Periods & menstrual health

What is severe period pain?
Periods & menstrual health

What are heavy periods?
Periods & menstrual health
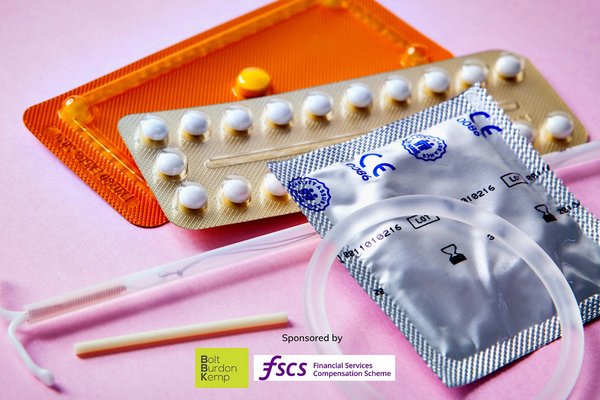
Contraception
Fertility

What is adenomyosis?
Periods & menstrual health

What is incontinence?
Incontinence

What is the menopause?
Perimenopause & menopause

What is endometriosis?
Periods & menstrual health

What are fibroids?
Periods & menstrual health
There are no health information pages.