
Rare, but deadly: tackling placental cancer
Vaginal cancer is a cancer that starts in the vagina. It’s a rare cancer, with only 250 cases diagnosed each year in the UK.

This cancer starts in the vagina. The vagina is the skin tube leading from the external genitalia (vulva) to the cervix (neck) of the womb.
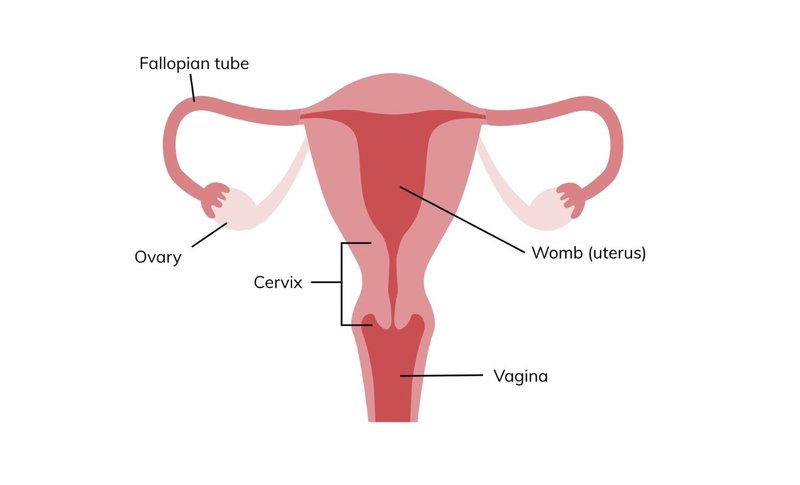
Vagina cancers occur when the cells forming the vagina start behaving abnormally and growing uncontrollably. There are many different types of vaginal cancer, because there are many different cell types that form the vagina. The specific type of cancer will depend on which cell type the cancer originated in.
Many cancers can spread to the vagina, but this is not the same as cancers that start in the vagina.
You can read about the different types of vaginal cancer here.
Vaginal cancer is rare. There are 250 new cases in the UK each year and it is more common in older people. Just over a third of new cases are in women aged 75 and over.
More than half of vaginal cancers are caused by an infection of high-risk human papillomavirus (HPV).
HPV is the name given to a group of viruses with more than 100 different types. Not all of them are cancer causing, the ones that can cause cancer are known as high-risk HPV.
HPV is common and most people will get the HPV virus at some point in their life. It’s spread through close skin-to-skin contact during any type of sexual activity with a partner.
Most of us won’t realise we have HPV. It can stay at very low or undetectable levels for many years without causing problems. In most cases, the body’s immune system will eliminate the virus within two years. This means an HPV infection may have come from a partner a long time ago.
Some types of HPV can cause genital warts, and women who have had genital warts are at an increased risk of developing a pre-cancer (VAIN).
You can protect yourself by attending cervical screening and with the HPV vaccine, which is offered to 12–13 year olds.
There are several things that may increase your risk of developing vaginal cancer:
Find out more about risk factors on the NHS website.
Anything that can reduce your risk of getting HPV and that supports your immune system to clear it if you do can help to reduce your risk of vaginal cancer. You can reduce your risk of vaginal cancer by:
It’s estimated that 75% of vaginal cancers can be prevented.
Symptoms of vaginal cancer can include:
You should go and see your GP if you have any of these symptoms. Even though these symptoms are unlikely to be vaginal cancer, it is still important to get checked.
Your doctor will ask you about your symptoms and examine you. They may refer you to the hospital for more tests. If you’re referred, you should have an appointment within two weeks.
It’s a good idea to keep a diary of your symptoms to take to any GP or hospital appointments. You may also want someone to go with you for support.
At the hospital you may have other tests such as:
The cancer may be staged and graded to help inform the treatment plan. This describes the size, whether it has spread and the changes in the cells. Find out more about staging and grading on the Macmillan website.
There are treatments for vaginal cancer that can remove the cancer and help stop it coming back. The treatment you have depends on the size of the cancer, how far it has spread and your overall health.
Treatments include surgery and radiotherapy.
If you’re diagnosed with vaginal cancer, your doctor will discuss the different treatments with you. You’ll also be able to ask them any questions that you might have.
It’s a good idea to discuss what your options are, and the benefits and risks of each, so that you can reach a decision that is best for you.
Worries about a possible diagnosis or living with cancer can be very challenging. Sometimes it can help to speak to people who understand and have experience of a vaginal cancer diagnosis.
You can read Val’s story of vaginal cancer.
You can find more information about vaginal cancer on the NHS website.
If you are worried about vaginal cancer or have been diagnosed with it, there are places to get support:
Watch again: Preventing gynae cancers webinar
In our latest webinar, we asked, can we prevent gynaecological cancer? We discussed the symptoms, how to reduce your risk, screenings that are available, and how to make sure screenings are accessible to all.You can also watch our previous webinars on gynaecological cancers, which feature experts and people with lived experience:
Let’s talk gynaecological (gynae) cancers – with Dr Neil Ryan and Sbba Siddique
Let's talk gynaecological cancers webinar – with Dr Sarah Kitson
As a women’s health charity, part of what we do is fund research to save and change the lives of women, girls and babies.







Finding the right information and support about gynaecological cancers can feel difficult, especially if you face barriers because of language, disability or a lack of tailored resources.

Cervical cancer develops in the cervix. This is the opening of the womb (uterus) into the vagina. There are over 3,200 cases diagnosed every year in the UK.

Ovarian cancer is cancer of the ovaries or fallopian tubes. Around 7,500 women get ovarian cancer in the UK each year.