
Rare, but deadly: tackling placental cancer
Most womb cancer starts in the lining of the uterus (womb). Around 9,700 women are diagnosed with womb cancer each year in the UK.

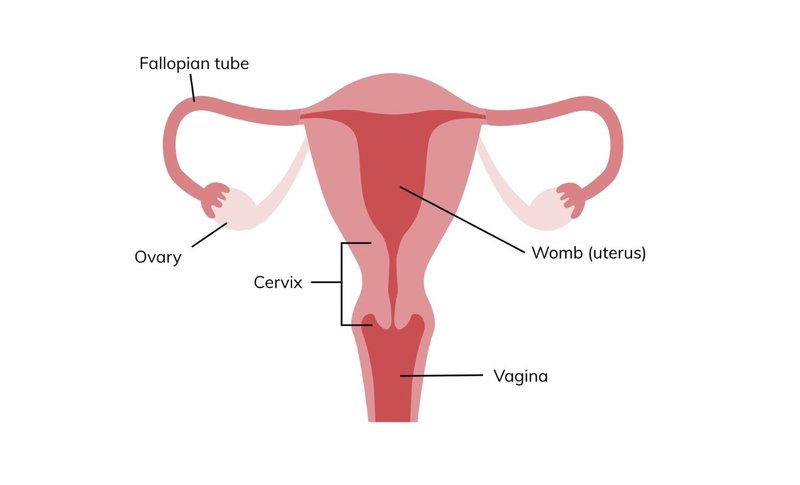
Most womb cancer starts within the lining of the womb (called the endometrium). The lining of the womb is shed every month during a period. The womb is an organ in the pelvis which is where a baby grows during pregnancy.
Most womb cancers occur when cells lining the womb start behaving abnormally and grow uncontrollably.
There are two main types of womb cancer defined by where the cancer starts:
Most womb cancers start in the endometrium. In these cases, it is sometimes referred to as ‘endometrial cancer’. There are a few different types of endometrial cancer, some more common and some rarer.
Uterine sarcomas are much rarer and require different treatments from endometrial cancers. If you’d like to know more about these cancers see the Cancer Research UK website.
Womb cancer is the fourth most common cancer in women in the UK. Around 9,700 women are diagnosed with womb cancer each year.
It’s not always clear why someone gets womb cancer. Having a high level of a hormone called oestrogen, without adequate balance of another hormone (called progesterone), can increase your risk.
You may have unbalanced oestrogen if you:
You might also be more likely to get womb cancer if you have:
You can reduce your risk of womb cancer by:
It’s estimated that 34% of womb cancers are preventable.
The most common symptom of womb cancer is bleeding from the vagina that is unusual for you.
This might be:
Other symptoms of womb cancer include:
Your symptoms might not be womb cancer and there are many other conditions that cause similar symptoms. One in 10 people who have bleeding after the menopause have womb cancer so it’s important to get checked by your GP. Finding womb cancer early makes it easier to treat.
Your doctor will ask you some questions about your symptoms. It’s a good idea to keep notes about your symptoms and take these with you to any GP or hospital appointments.
They may also want to do a physical examination which could involve:
Your GP may send you for an ultrasound scan. If this shows that the lining of the womb is thickened, you will need to see a gynaecological specialist to have a sample (biopsy) taken from the lining of the womb. You may want someone to go with you to your appointment for support.
The NHS has more information about the tests you may have.
The cancer may be staged and graded to help inform the treatment plan. This describes the size, whether it has spread and the changes in the cells. Find out more about staging and grading on the Macmillan website.
There are a few different treatments for womb cancer. The treatment you will have will depend on the type of the cancer and if it’s spread. Treatments can include:
Most womb cancers are found at an early stage and can be treated with surgery to remove the womb – this is called a hysterectomy. This means you are no longer able to get pregnant. It often involves removing the ovaries and fallopian tubes too.
Some types of womb cancer can respond well to hormone treatment. If you are at very high risk for an anaesthetic/surgery, hormone treatment may provide time for interventions to reduce your risks before going ahead with an operation, for example, treatment to help you lose weight.
In young women with the type of cancer that can respond well to hormone treatment, it may be possible to treat the cancer with hormones first. This may mean you can delay surgery and allow time to have a baby in the future. Ask your doctor if this is something you would consider.
It’s normal to fear cancer coming back after treatment. If you spot any symptoms, speak to your GP. The symptoms do not necessarily mean the cancer is back.
You can find out more information about womb cancer on the NHS website.
The charity Peaches Womb Cancer Trust provides support and information for those with and at risk of womb cancer. Go Girls supports women, men, trans people and non-binary people diagnosed with gynaecological cancer.
The charity The Eve Appeal has a guide for women about womb cancer. It also runs a nurse-led helpline and email support service, called Ask Eve.
Womb Cancer Support UK runs a private Facebook group for women affected by womb cancer.
Watch again: Preventing gynae cancers webinar
In our latest webinar, we asked, can we prevent gynaecological cancer? We discussed the symptoms, how to reduce your risk, screenings that are available, and how to make sure screenings are accessible to all.You can also watch our previous webinars on gynaecological cancers, which feature experts and people with lived experience:
Let’s talk gynaecological (gynae) cancers – with Dr Neil Ryan and Sbba Siddique
Let's talk gynaecological cancers webinar – with Dr Sarah Kitson
As a women’s health charity, part of what we do is fund research to save and change the lives of women, girls and babies.
We are currently funding a study to help healthcare professionals spot and treat women at risk of developing womb cancer.







Finding the right information and support about gynaecological cancers can feel difficult, especially if you face barriers because of language, disability or a lack of tailored resources.

Cervical cancer develops in the cervix. This is the opening of the womb (uterus) into the vagina. There are over 3,200 cases diagnosed every year in the UK.

Ovarian cancer is cancer of the ovaries or fallopian tubes. Around 7,500 women get ovarian cancer in the UK each year.