
Gynae cancer support and resources for marginalised groups
Finding the right information and support about gynaecological cancers can feel difficult, especially if you face barriers because of language, disability or a lack of tailored resources.
Cervical screening is a vital health check that helps prevent cervical cancer by detecting abnormal cells early. Here's everything you need to know about the test and why it’s crucial to your health.
Cervical screening checks the health of your cervix. The cervix is the lower part of the womb that connects to your vagina.
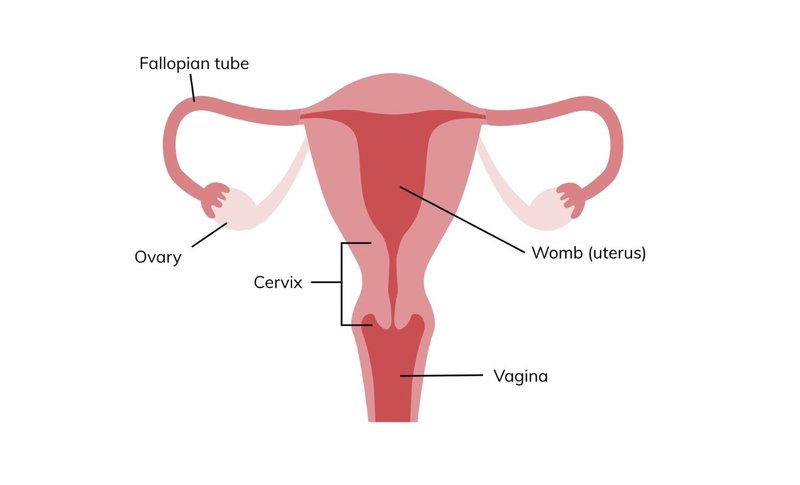
Screening involves collecting a small sample of cervical cells which are then tested.
Screenings check your cervix for a type of virus called high-risk human papillomavirus (HPV). This type of virus can cause cancer. If HPV is found, the cervical cells are then looked at to see if they are abnormal (if have any changes which could be pre-cancerous).
Cervical screening is not a test for cancer, but it can help prevent cancer by spotting any problems early. Screening is crucial as it helps to prevent cervical cancer.
You're automatically invited for screening if you are:
You will be invited to a screening every 5 years if you live in England, Wales or Scotland. In Northern Ireland, women between 25 and 49 are invited every 3 years and women aged 50 to 64 are invited every 5 years.
Once you turn 65, you will only be invited again if your last test was abnormal.
If you have symptoms of cervical cancer, like unusual bleeding from your vagina, pain or changes to discharge, you should speak to your GP as soon as possible and not wait until you’re invited to your next screening.
Sometimes cervical screening is referred to as a ‘smear test’. This comes from the older method of screening where a stick was used to collect cells, which were then smeared onto a plate for lab analysis. Nowadays, a brush is used, but the name is still sometimes used.
A doctor or nurse will carry out the test. The procedure is simple and takes around five minutes:
You can ask for someone else to be present if you would like. This is usually another health professional. You can also bring a friend, relative or carer with you.
You might find wearing a skirt or dress helpful.
You might experience slight bleeding afterwards, which is normal. You may want to bring a sanitary pad with you or wear period knickers.
The test can be painful for some, especially if you have a history of trauma.
Other things like vaginal dryness, vaginismus (involuntary tightening of the vaginal muscles) or lichen sclerosus may also make it more difficult.
If you’re anxious about being alone with your nurse, or want extra emotional support, you can take someone with you to the appointment. You can also ask for a longer appointment, so you can take the appointment at a pace that is more comfortable for you.
You can ask to insert the speculum yourself, if that would be more comfortable, and there are different sizes of speculum available.
A water-based lubricant can be used and won't affect the results. If this isn't available, you are within rights to leave the test, or you might like to bring your own lubricant with you.
If you are in the menopausal or perimenopausal stages, you could have vaginal atrophy (thinning and drying of the vagina). Your healthcare professional can prescribe topical vaginal oestrogen (applied directly to the vagina) as a pessary (removal device that is inserted into the vagina) or a cream at least three weeks prior to the smear test. This is then stopped two days before the test.
If it hurts or you are worried, let the person doing the test know so they can help. They’re used to this and can guide you through it.
It's best to avoid the test during your period. If you unexpectedly start your period, you can rebook. This is to ensure your comfort and also because red blood cells can sometimes disrupt the screening sample, making it hard to pick up on subtle changes in the cells.
You will not usually need to have cervical screening if you're pregnant, or could be pregnant, until at least 12 weeks after you've given birth. This is because pregnancy can make it harder to get clear results.
If you're pregnant and due for a cervical screening test, you will usually be advised to reschedule the test for a date after your baby is born.
If you've previously had an abnormal result from a cervical screening test, you may need to be screened while you're pregnant. Your GP or midwife will discuss any risks with you and arrange a screening if needed.
The HPV vaccine helps to protect against cancers caused by HPV and is given as one injection.
Boys and girls are offered the vaccine between 12 and 13 years old.
The vaccine does not protect against all subtypes of HPV, so you should still attend your screening, even if you’ve had a vaccination.
Talking to friends and family who have undergone screening can help alleviate anxiety. Sharing positive experiences can be reassuring. Consider practicing relaxation techniques or speaking with your clinician about your concerns. Discussing how to make the screening more comfortable with your doctor or nurse may help.
HPV is very common and most people will contract it at some point in their lives. It is not usually treated, because it often clears up on its own. Regular cervical screenings are important to monitor any potential cell changes caused by HPV.
The person doing your screening should tell you when to expect your results.
Possible results from a screening are:
If abnormal cells are found, it’s important to remember that they are not cancer, but there is a risk they could become cancerous. That's why it's important to have a follow up check and monitor any changes.
If your cervical screening results are negative for HPV, but you have any symptoms you’re worried about, you should speak to your GP. They can assess you and refer you for further tests if necessary.
There are plans for an HPV test that can be done yourself to be made available through the NHS. This test will enable people who have rarely or never attended their cervical screening to take a sample at home (self-sample).
The test will check for the presence of HPV, but it will not be able to detect whether there are any abnormal cells. If the test shows you have HPV, you will need to have a normal cervical screening, so your cervical cells can be looked at.
The test is due to be rolled out across England from early 2026. Roll out is expected in Wales and Scotland in 2026. In Northern Ireland, the test is being considered for use.
Self-sampling will only be offered to select groups of women who have never or rarely had a screening.
Regular cervical screenings are vital for early detection and prevention of cervical cancer. Since the screening programme started, the number of women dying from cervical cancer has halved.
Although it can be uncomfortable, and sometimes painful, regular cervical screenings are important to ensure any problems are caught early.
Learn more about cervical cancer, including how it is treated, on our cervical cancer page.

Finding the right information and support about gynaecological cancers can feel difficult, especially if you face barriers because of language, disability or a lack of tailored resources.

Cervical cancer develops in the cervix. This is the opening of the womb (uterus) into the vagina. There are over 3,200 cases diagnosed every year in the UK.

Ovarian cancer is cancer of the ovaries or fallopian tubes. Around 7,500 women get ovarian cancer in the UK each year.