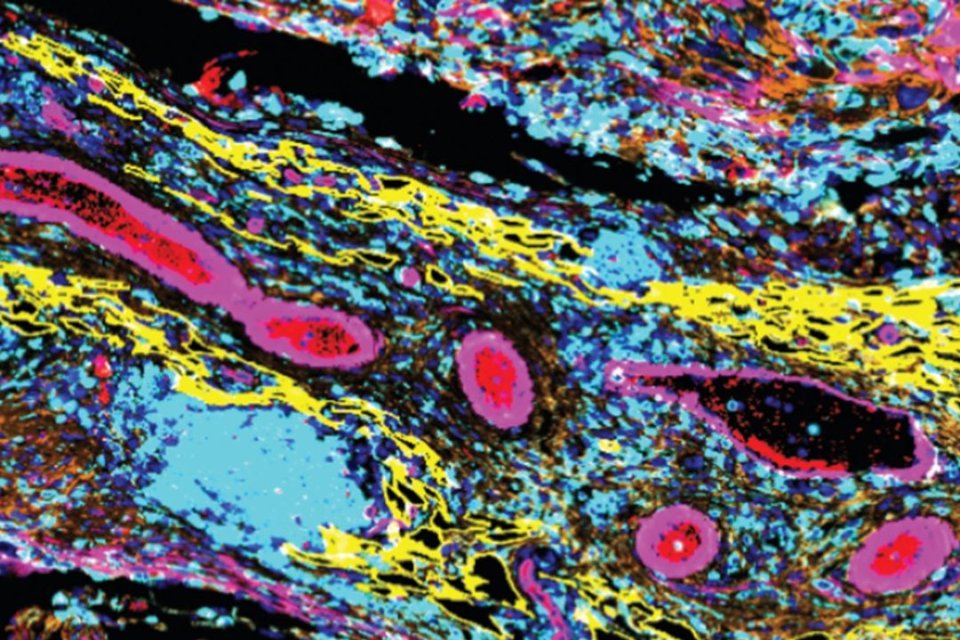
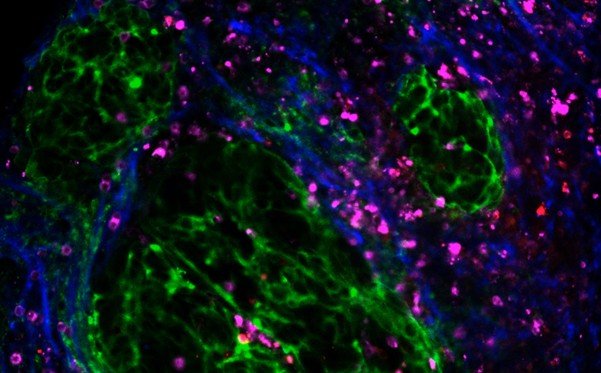
Unlocking the cellular structure of ovarian cancer tumours
Wellbeing of Women, in partnership with the British Gynaecological Cancer Society (BGCS), are funding new work by Dr Shimrit Mayer at the CRUK Cambridge Institute on improving the outlook for ovarian cancer patients