
Rare, but deadly: tackling placental cancer
Cervical cancer develops in the cervix. This is the opening of the womb (uterus) into the vagina. There are over 3,200 cases diagnosed every year in the UK.

Cervical cancer affects your cervix, which is part of the female reproductive system. It is sometimes called the neck or opening of the womb.
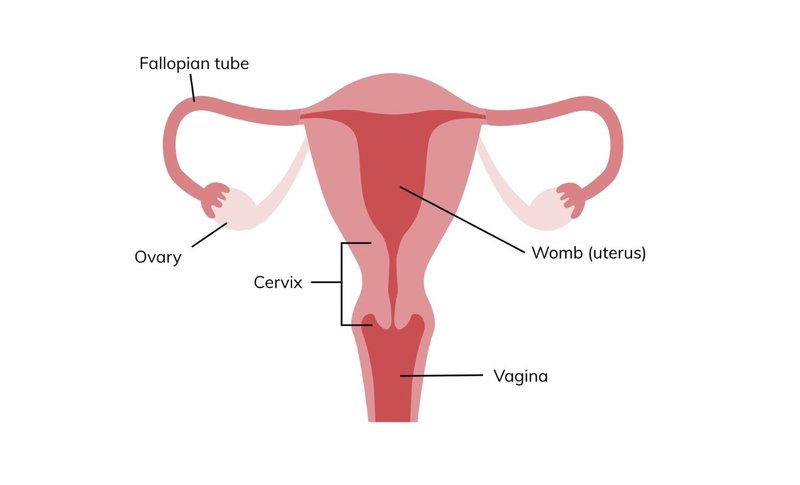
Cervical cancer happens when cells in the cervix start growing irregularly and multiply uncontrollably.
There are two main types of cervical cancer: squamous cell cancer and adenocarcinoma. These are named after the type of cell that becomes cancerous.
Cervical cancer usually grows slowly. In people with healthy immune systems, it typically takes 15-20 years for cervical cancer to develop.
Cervical cancer begins with changes occurring in cells. These are known as abnormal cells, and they can be graded by how abnormal they are.
Sometimes, abnormal cells are destroyed by the body, so no action is needed. These are known as borderline or low-grade changes.
However, sometimes, the body is unable to deal with these cells, and they can go on to develop into cancer. These abnormal cells are referred to as pre-cancerous and are known as high grade changes.
It may be helpful to familiarise yourself with the difference between the classifications of pre-cancer, the difference between pre-cancer and cancer and the different stages of cervical cancers.
There are over 3,200 cases of cervical cancer in the UK each year. Cervical cancer rates in the UK are highest in women and people with a cervix aged 30–34 years. But younger and older women can still get cervical cancer so it’s important you attend screening appointments.
Nearly all cervical cancers are caused by the human papillomavirus (HPV). HPV is the name given to a group of viruses with more than 100 different types. Not all of them are cancer causing, the ones that can cause cancer are known as high-risk HPV. HPV is very common, and most people will get the virus at some point in their life.
HPV is spread through close skin-to-skin contact during any type of sexual activity with a partner.
Most of us won’t realise we have HPV. It can stay at very low or undetectable levels for many years without causing problems. In most cases, the body’s immune system will eliminate the virus within two years. This means an HPV infection may have come from a partner a long time ago.
Although almost all cases of cervical cancer are caused by HPV, there are other risk factors that can increase the risk of developing cervical cancer:
Anything that can reduce your risk of getting HPV and that supports your immune system to clear it if you do can help to reduce your risk of cervical cancer. You can reduce your risk of developing cervical cancer by:
It’s estimated that 99.8% of cervical cancers are preventable.
Cervical cancer often has no symptoms in its early stages. Most people are diagnosed through the NHS cervical screening programme. That’s why cervical screening is so important.
The most common symptoms of cervical cancer are:
If you have these symptoms speak to your GP, don’t wait for your next screening appointment.
Screening is one of the best ways to protect yourself from cervical cancer. Since screening started, the number of women dying from cervical cancer has halved.
Also known as a smear test, cervical screening checks the health of your cervix. It checks for high-risk HPV and if positive, the cells are looked at to see if they are pre-cancerous. It’s not a test for cancer, but it can help prevent cancer by spotting any problems early.
You’re automatically invited for screening if you’re:
Trans men do not receive invitations if registered as male with their GP but are still entitled to screening if they have a cervix. Make sure you speak to your GP and ensure you are invited for screening if this applies to you.
Cervical cancer can spread to other areas of the body. That’s why it’s important to always attend your screening appointments to spot it early.
Find out more about cervical cancer screening.
The HPV vaccine helps to protect against cancers caused by HPV and is given as one injection.
Boys and girls are offered the vaccine between 12 and 13 years old (Year 8 at school), but if they miss it for any reason, they can still get it for free on the NHS until their 25th birthday if:
The NHS website also has lots of information about the HPV vaccine.
If your smear test found signs of abnormal cells or if you spoke to your GP about possible symptoms, you’ll have some tests.
The most common test is a colposcopy. A speculum will be placed into the vagina to enable the colposcopist to see your cervix, and a microscope with a light at the end is used to study the cervix in more detail (the microscope isn’t inserted into the vagina). The colposcopist may apply some dye to the cervix to help highlight any abnormal cells.
Depending on the result, you may have some other tests, including:
During diagnosis, the cancer may be staged, which indicates the size and whether it has spread, and helps to inform the treatment plan. Find out more about cervical cancer staging on the Macmillan website.
There are different treatments for cervical cancer. The best treatment for you will depend on the type, grade and stage of cervical cancer you have, how big the tumour is and if it has spread.
Treatments for cervical cancer include:
If you are diagnosed with cervical cancer, it is likely that you will receive a combination of these treatments. Your doctor can discuss the options with you, and you’ll be able to ask them any questions that you might have.
It’s a good idea to discuss what your options are and the benefits and risks of each so that you can reach a decision that is best for you. Sometimes appointments can feel overwhelming, so it can be helpful to write down your questions in advance and take a second person along or ask if you can record the appointment.
For more information about cervical cancer treatments, visit the NHS website.
Cervical cancer is often treatable, but this can depend on how early the cancer is detected. As with all cancers, catching it early makes it easier to treat. That’s why it’s important to attend your screening appointments and go to your GP if you spot any symptoms.
Worries about a possible diagnosis or living with cancer can be very challenging. Sometimes it can help to speak to people who understand and have experience of a cervical cancer diagnosis.
You can read Aoife’s story of cervical cancer.
If you’d like more information or support for a cervical cancer diagnosis, there are places you can go to get support.
These organisations have more information and support:
Watch again: Preventing gynae cancers webinar
In our latest webinar, we asked, can we prevent gynaecological cancer? We discussed the symptoms, how to reduce your risk, screenings that are available, and how to make sure screenings are accessible to all.You can also watch our webinars on gynaecological cancers, which feature experts and people with lived experience:
As a women’s health charity, we fund research to save and change the lives of women, girls and babies.
Our research played a part in establishing the link between HPV and cervical cancer, resulting in the first preventative school-wide vaccination programme.
And we are currently co-funding a research study with the British Gynaecological Cancer Society to investigate if an innovative new technology can help detect and treat cervical and vulval cancers faster and more accurately.







Finding the right information and support about gynaecological cancers can feel difficult, especially if you face barriers because of language, disability or a lack of tailored resources.

Ovarian cancer is cancer of the ovaries or fallopian tubes. Around 7,500 women get ovarian cancer in the UK each year.

Most womb cancer starts in the lining of the uterus (womb). Around 9,700 women are diagnosed with womb cancer each year in the UK.