Research projects
We are proud to work with some of the UK’s top doctors, midwives, nurses and scientists to make the greatest difference to the lives of women and their families.
Spanning across the lifecourse – periods & menstrual health, pregnancy and birth, fertility, contraception & abortion care, gynaecological cancers, sexual health & wellbeing, gynaecological conditions, pelvic floor health, perimenopause & menopause, and post menopause – here is some of our work.

Understanding at the source: the womb, endometriosis and how blood works
Current projects
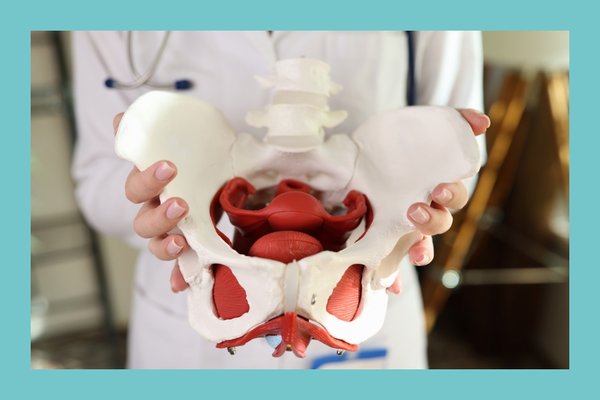
Pain and pelvic mesh: Wellbeing of Women invests £160,000 in Dr Joseph O’Sullivan’s PhD on possible causes of mesh pain
Current projects

Attitudes to contraception in the UK: ethnic minority and religious perspectives
Our impact
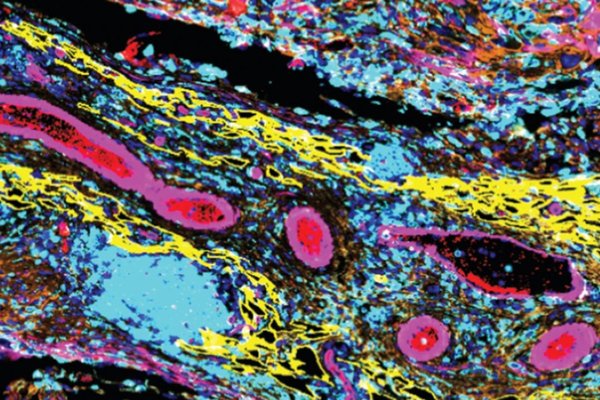
Women’s health highlight: Improving the effects of chemotherapy for ovarian cancer?
Our impact

Unlocking the cellular structure of ovarian cancer tumours
Current projects

‘Being under’ during birth: Improving care for people who experience caesarean section birth with general anaesthetic
Current projects

Rare, but deadly: tackling placental cancer
Current projects
Engineering new treatments for ovarian cancer
Current projects

Preventing womb cancer: new tools offer new hope
Our impact
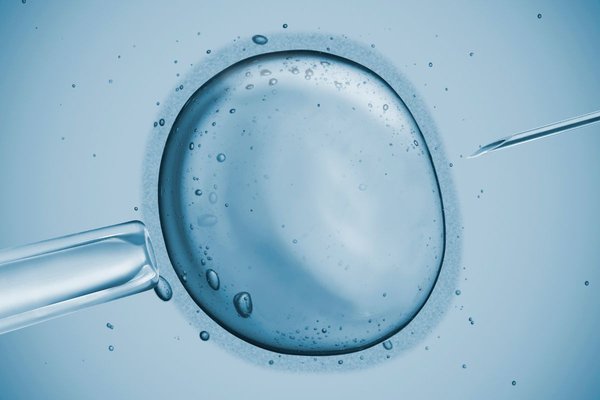
What matters most in female fertility preservation?
Current projects

Predicting the future: could a new genetic tool help us improve ovarian cancer outcomes?
Current projects

Women's Health Highlight: Dr Nicola Tempest on stem cells, the womb and the future of fertility
Our impact
There are no articles.